A sleep study, also known as polysomnography (PSG), is a diagnostic test used to evaluate sleep disorders and abnormalities in sleep patterns. It involves monitoring various physiological parameters during sleep, including brain activity, eye movements, muscle tone, respiratory effort, airflow, oxygen saturation, and heart rate. The data collected during a sleep study provide valuable information about sleep architecture, the presence of sleep-related breathing disorders, and other sleep disorders.
Types of Sleep Studies
There are several types of sleep studies, each tailored to evaluate specific aspects of sleep and diagnose different sleep disorders. The main types of sleep studies include:
- Polysomnography (PSG): PSG is the most comprehensive type of sleep study, conducted in a sleep laboratory or clinic. It involves monitoring multiple physiological parameters during an overnight stay, including electroencephalography (EEG) to measure brain activity, electrooculography (EOG) to monitor eye movements, electromyography (EMG) to assess muscle tone, and other sensors to monitor respiratory and cardiovascular parameters.
- Home Sleep Apnea Test (HSAT): HSAT, also known as a home sleep study or portable sleep study, is a simplified version of PSG that can be conducted in the patient’s own home. It typically involves monitoring respiratory parameters, such as airflow, respiratory effort, and oxygen saturation, using a portable device worn by the patient while sleeping.
- Multiple Sleep Latency Test (MSLT): MSLT is a daytime sleep study used to evaluate excessive daytime sleepiness and diagnose narcolepsy and other hypersomnias. It involves monitoring the patient’s tendency to fall asleep during multiple short nap opportunities throughout the day, typically following an overnight PSG.
- Maintenance of Wakefulness Test (MWT): MWT is a daytime sleep study used to assess the patient’s ability to stay awake and alert during periods of wakefulness. It is often used to evaluate daytime alertness and assess treatment response in patients with sleep disorders such as narcolepsy or sleep apnea.
Procedure
The procedure for a sleep study varies depending on the type of study being conducted, but the general process for an overnight PSG in a sleep laboratory typically includes the following steps:
- Preparation: The patient arrives at the sleep laboratory in the evening and is prepared for the sleep study by a sleep technologist or healthcare provider. Electrodes and sensors are applied to the patient’s scalp, face, chest, legs, and other body parts to monitor physiological parameters during sleep.
- Monitoring: The patient is allowed to sleep in a comfortable bed in a quiet, dimly lit room while the sleep technologist monitors the recordings from the control room. Throughout the night, the sleep technologist observes the patient’s sleep patterns and adjusts the sensors as needed to ensure optimal data collection.
- Data Collection: During the sleep study, multiple physiological parameters are recorded continuously, including brain activity (EEG), eye movements (EOG), muscle tone (EMG), respiratory effort, airflow, oxygen saturation, and heart rate. The recordings are stored electronically for later analysis by a sleep specialist.
- Morning Evaluation: In the morning, the patient is awakened, and the sensors and electrodes are removed. The patient may be asked to complete a questionnaire about their sleep experience during the study. The recorded data are then analyzed by a sleep specialist to evaluate sleep architecture, detect abnormalities or sleep disorders, and formulate a diagnosis and treatment plan.
Indications
Sleep studies may be indicated for patients with signs and symptoms suggestive of sleep disorders, including:
- Excessive daytime sleepiness
- Loud snoring
- Witnessed apneas or gasping during sleep
- Restless legs syndrome
- Insomnia
- Unexplained awakenings or sleep disturbances
- Abnormal behaviors during sleep (e.g., sleepwalking, night terrors)
Sleep machines are commonly used to assist individuals with various sleep-related issues, especially for conditions like obstructive sleep apnea (OSA) and insomnia. Here are the primary uses of sleep machines:
1. Home Sleep Testing Devices
- Purpose: Portable machines for diagnosing sleep apnea and other sleep disorders at home.
- Benefits:
- Convenient and less expensive than in-lab testing.
- Tracks parameters like breathing, oxygen levels, and heart rate.
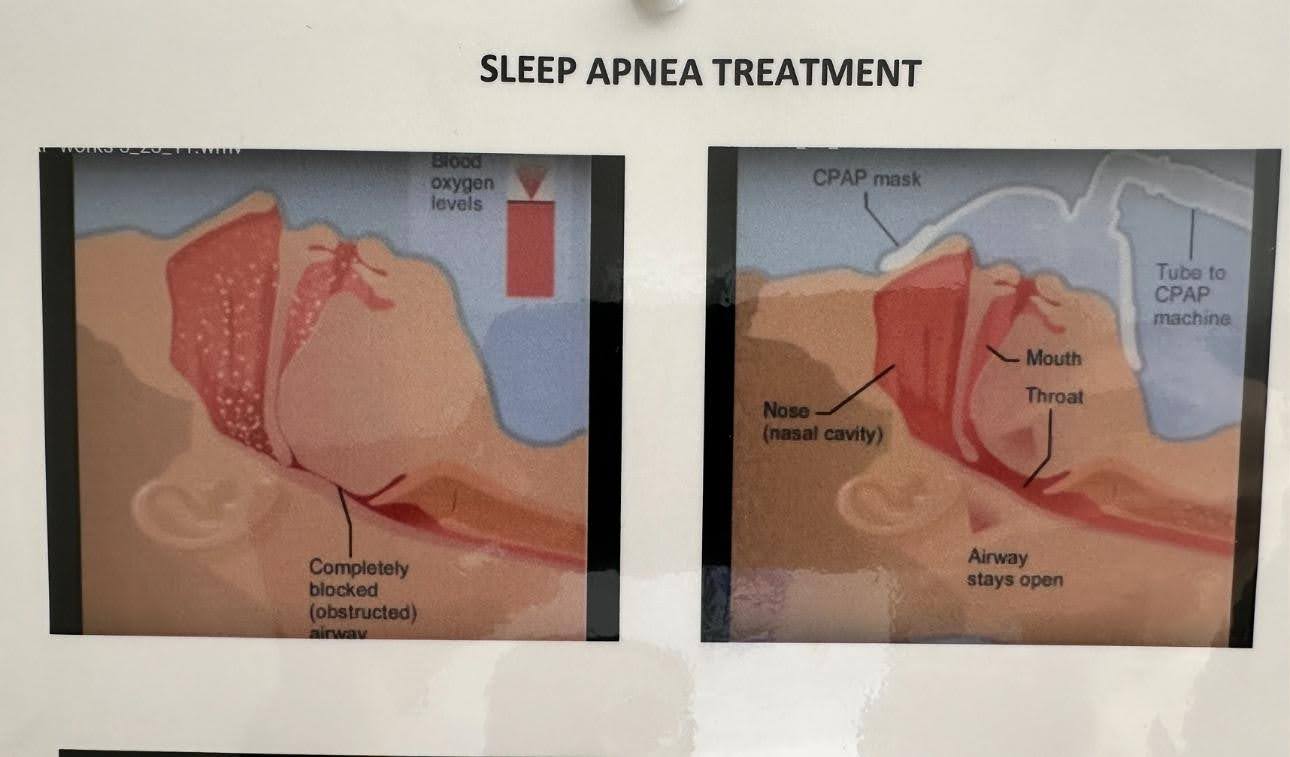
2. CPAP Machines for Sleep Apnea
- Purpose: Continuous Positive Airway Pressure (CPAP) machines are used to keep the airway open during sleep by delivering a constant stream of air.
- Benefits:
- Prevents airway collapse.
- Reduces snoring and improves sleep quality.
- Lowers risk of complications such as heart disease, high blood pressure, and stroke.
- Common Features:
- Adjustable pressure settings.
- Humidification to reduce dryness.
- Mask types to suit individual preferences (nasal, full-face, etc.).
3. BiPAP Machines
- Purpose: Bilevel Positive Airway Pressure (BiPAP) machines provide different pressure levels for inhalation and exhalation, often for more severe cases of apnea or other respiratory conditions.
- Benefits:
- Easier breathing during exhalation.
- Helps with conditions like central sleep apnea and COPD.
Benefits
The benefits of sleep studies include:
- Accurate Diagnosis: Sleep studies provide valuable diagnostic information about sleep architecture, respiratory events, and other sleep abnormalities, allowing for accurate diagnosis and targeted treatment of sleep disorders.
- Treatment Guidance: The results of sleep studies help guide treatment decisions, including the use of continuous positive airway pressure (CPAP) therapy for sleep apnea, medications for insomnia or restless legs syndrome, and behavioral therapies for sleep-related disorders.
- Improved Quality of Life: Effective treatment of sleep disorders based on the results of sleep studies can lead to improved sleep quality, daytime functioning, and overall quality of life for patients.
Risks and Considerations
Sleep studies are generally safe, non-invasive, and well-tolerated by most patients. However, there are some risks and considerations to be aware of, including:
- Discomfort: Some patients may find the sensors and electrodes used during the sleep study to be uncomfortable or disruptive to sleep.
- Inconvenience: Sleep studies typically require an overnight stay in a sleep laboratory or wearing a portable device at home, which may be inconvenient for some patients.
- Incomplete Data: Sleep studies may not capture all aspects of sleep architecture or detect all sleep-related abnormalities, particularly in patients with intermittent or complex sleep disorders.
Conclusion
Sleep studies, including polysomnography (PSG) and other specialized tests, play a crucial role in the diagnosis and management of sleep disorders by providing valuable information about sleep architecture, respiratory events, and other physiological parameters during sleep. When conducted by trained sleep technologists and interpreted by sleep specialists, sleep studies help guide treatment decisions, improve sleep quality, and enhance overall health and well-being for patients with sleep disorders.