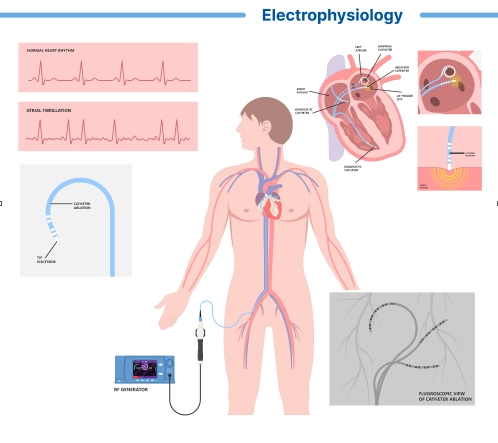
An electrophysiology (EP) study is a specialized cardiac procedure used to evaluate the electrical activity of the heart and diagnose or treat abnormal heart rhythms or arrhythmias. It involves inserting catheters into the heart to record electrical signals, map the heart’s conduction system, and induce and terminate arrhythmias for diagnostic or therapeutic purposes.
Procedure
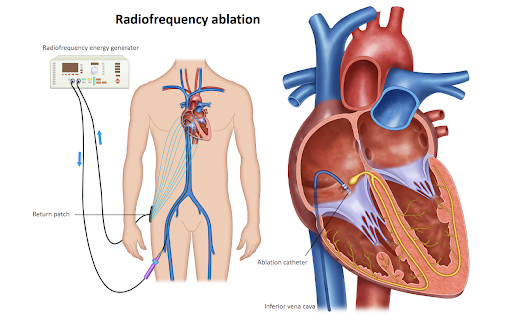
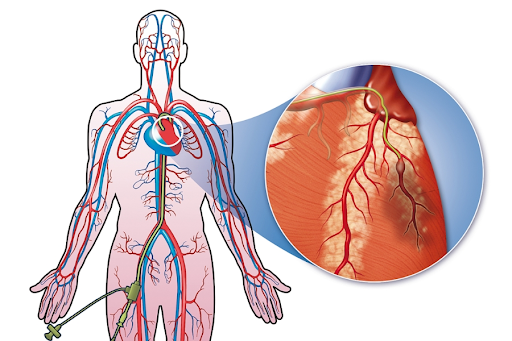
During an EP study, the patient is typically awake but sedated to help them relax. The procedure is performed in a specialized cardiac electrophysiology laboratory (EP lab) by a team of cardiac electrophysiologists and nurses. The following steps outline the general process of an EP study:- Access: The cardiologist inserts one or more catheters (thin, flexible tubes) into a blood vessel, usually in the groin or neck, using a small needle and guide wire. Local anesthetic is applied to numb the insertion site.
- Guidance: The catheters are advanced through the blood vessel and guided to the heart using X-ray imaging (fluoroscopy) and, in some cases, three-dimensional mapping systems. This allows the cardiologist to position the catheters in specific areas of the heart and record electrical signals.
- Recording: Once the catheters are positioned within the heart, they are used to record electrical signals from various areas of the heart, including the atria, ventricles, and specialized conduction pathways. The recorded signals are displayed on a monitor and analyzed to assess the heart’s electrical activity.
- Stimulation: In some cases, the cardiologist may use the catheters to deliver electrical impulses to the heart to induce or provoke arrhythmias. This allows for diagnostic assessment of the heart’s response to different pacing protocols and helps identify the underlying mechanisms of arrhythmias.
Uses of EP Study
EP studies are used for various diagnostic and therapeutic purposes, including:- Diagnosing Arrhythmias: EP studies help diagnose the type, location, and mechanism of arrhythmias, including atrial fibrillation, supraventricular tachycardia, ventricular tachycardia, and other complex arrhythmias.
- Assessing Risk: EP studies help assess the risk of sudden cardiac death and other adverse cardiovascular events in patients with certain arrhythmias or structural heart disease.
- Guiding Treatment: EP studies guide treatment decisions for arrhythmias, including selection of antiarrhythmic medications, implantable devices (such as pacemakers or implantable cardioverter-defibrillators), and catheter ablation procedures.
- Evaluating Treatment Response: EP studies assess the effectiveness of treatments for arrhythmias and monitor changes in the heart’s electrical activity over time.
Risks and Considerations
EP studies are generally safe, but they carry some risks and considerations, including:- Bleeding: Bleeding or hematoma at the insertion site is a common complication of EP studies.
- Vascular Injury: Rarely, EP studies can cause injury to blood vessels, leading to bleeding, hematoma, or pseudoaneurysm formation.
- Arrhythmia Induction: Inducing arrhythmias during the EP study carries a risk of triggering potentially dangerous arrhythmias or complications, particularly in patients with underlying heart disease.
- Radiation Exposure: EP studies involve exposure to ionizing radiation from X-ray imaging, which carries a small risk of radiation exposure for patients and healthcare providers.