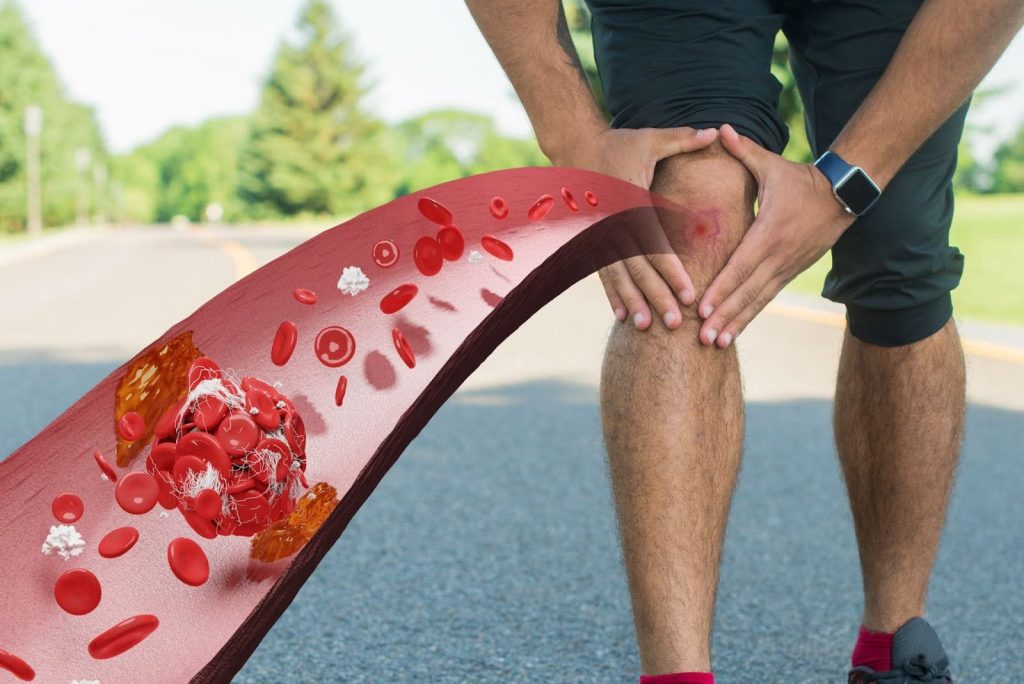
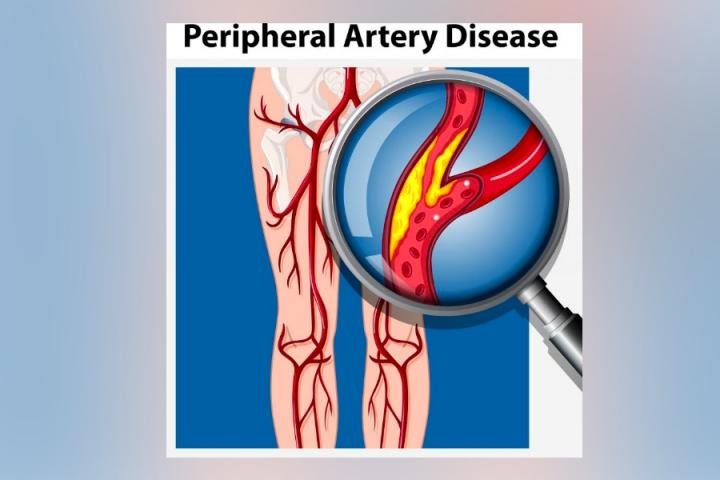
Peripheral Artery Disease (PAD) is a common circulatory problem in which narrowed arteries reduce blood flow to the limbs, usually the legs. PAD is typically caused by atherosclerosis, a condition where fatty deposits (plaque) build up on the walls of the arteries, narrowing them and restricting blood flow.
Causes and Risk Factors
The primary risk factors for developing PAD include:- Smoking: The most significant risk factor for PAD; tobacco use damages the blood vessels and increases the risk of atherosclerosis.
- Diabetes: High blood sugar levels can damage the arteries and contribute to the development of PAD.
- High blood pressure (hypertension): Increases the risk of atherosclerosis and can accelerate the progression of PAD.
- High cholesterol: Elevated levels of LDL (“bad”) cholesterol can lead to the accumulation of plaque in the arteries.
- Age: PAD is more common in older adults, particularly those over 50.
- Family history: Individuals with a family history of PAD or other cardiovascular diseases have an increased risk.
- Obesity: Excess weight puts additional strain on the circulatory system and increases the risk of atherosclerosis.
- Inactive lifestyle: Lack of regular exercise can contribute to the development and progression of PAD.
Symptoms
Many people with PAD may not experience any symptoms, especially in the early stages. However, as the condition progresses, symptoms may include:- Leg pain: Typically cramping or muscle pain in the legs, especially during physical activity (intermittent claudication). Pain often subsides with rest.
- Numbness or weakness: In the legs.
- Coldness or changes in skin color: Particularly in the feet or legs.
- Poor wound healing: Sores or wounds on the legs or feet that heal slowly or poorly.
- Weak or absent pulses: In the feet or legs.
Diagnosis
Diagnosis of PAD may involve:- Physical examination: Checking for signs of poor circulation, including weak pulses, cool skin, and wounds that heal slowly.
- Ankle-brachial index (ABI): Comparing blood pressure measurements in the arms and ankles to assess blood flow to the legs.
- Doppler ultrasound: Using sound waves to create images of blood flow in the arteries.
- Angiography: Injecting dye into the arteries and taking X-rays to visualize blood flow and any blockages.
Treatment
Treatment for PAD aims to relieve symptoms, prevent complications, and improve blood flow. Treatment options may include:- Lifestyle changes: Such as smoking cessation, regular exercise, and a healthy diet low in saturated fats.
- Medications: Including antiplatelet drugs, cholesterol-lowering medications, and medications to manage symptoms such as pain or high blood pressure.
- Peripheral angioplasty and stenting: Procedures to open blocked arteries and improve blood flow.
- Peripheral artery bypass surgery: Surgery to create a new route for blood flow around a blocked artery.
Prevention
Prevention strategies for PAD include:- Healthy lifestyle habits: Including regular exercise, maintaining a healthy weight, and eating a balanced diet.
- Managing underlying health conditions: Such as diabetes, high blood pressure, and high cholesterol.
- Avoiding tobacco: Smoking cessation is crucial for preventing and managing PAD.
