Source Link: https://www.ncbi.nlm.nih.gov/books/NBK441860/
The Long QT Syndrome (LQTS) is a heart rhythm disorder that can potentially lead to fast, chaotic heartbeats. These rapid heartbeats might trigger a sudden fainting spell or seizure. In some cases, the heart may beat erratically for so long that it can cause sudden death.
Causes:
LQTS can be congenital (inherited) or acquired due to certain medications or medical conditions. The disorder is characterized by a prolongation of the QT interval, which is a specific measurement made on an electrocardiogram (ECG) reflecting the time it takes for the heart’s electrical system to recharge between beats. Here’s more on the causes:
- Congenital LQTS : Often caused by genetic mutations affecting ion channels in the heart. These channels control the flow of ions in and out of heart cells, affecting how the heart beats.
- Acquired LQTS : Can be induced by certain medications (such as certain antibiotics, antihistamines, diuretics, antidepressants, and drugs used to treat arrhythmias), electrolyte imbalances (like low potassium or magnesium), or medical conditions that affect the heart.
Symptoms:
Symptoms of LQTS can vary significantly from person to person, even among family members with the condition. Common symptoms include:
- Fainting (syncope), often triggered by exercise, stress, or sudden fright.
- Seizures
- Palpitations
- Sudden cardiac arrest in severe cases
Diagnosis:
Diagnosis of LQTS typically involves:
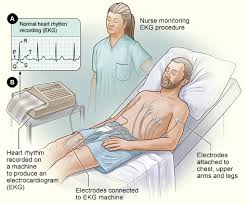
- Electrocardiogram (ECG): To measure the QT interval and detect other abnormalities.
- Holter monitoring: A portable device is worn to record a continuous ECG, usually for 24-48 hours, to detect intermittent arrhythmias.
- Event recorder: A device worn for weeks to months to record the heart’s activity over a long period.
- Genetic testing: Can identify specific mutations in genes related to LQTS, which is particularly useful for screening family members.
- Exercise stress test: To observe the heart’s activity during physical exertion.
Treatment:
Treatment for LQTS aims to prevent the abnormal heart rhythms associated with the condition:
- Beta-blockers: These are the mainstay treatment for patients with LQTS, as they slow the heart rate and reduce the likelihood of arrhythmias.
- Potassium supplements or other medications: These may be used to normalize heart function, particularly if the LQTS is associated with electrolyte imbalances.
- Implantable cardioverter-defibrillator (ICD): For patients at high risk of sudden cardiac death, an ICD can be implanted to provide immediate treatment for life-threatening arrhythmias.
- Lifestyle adjustments: Patients are often advised to avoid competitive sports, strenuous exercise, and other situations that may trigger a rapid heart rate. Awareness and avoidance of drugs known to prolong the QT interval are also critical.
Management:
Regular follow-up with a cardiologist experienced in managing LQTS is crucial. Family members of individuals diagnosed with congenital LQTS may also be advised to undergo genetic testing and ECG screenings due to the hereditary nature of the condition.
The QT interval on an electrocardiogram (ECG) represents the duration of the ventricular action potential, and this physiologically correlates with the duration of the ventricular depolarization and repolarization. Cardiac events and fatal arrhythmias may occur when the QT interval is prolonged either congenitally or through acquired causes.
