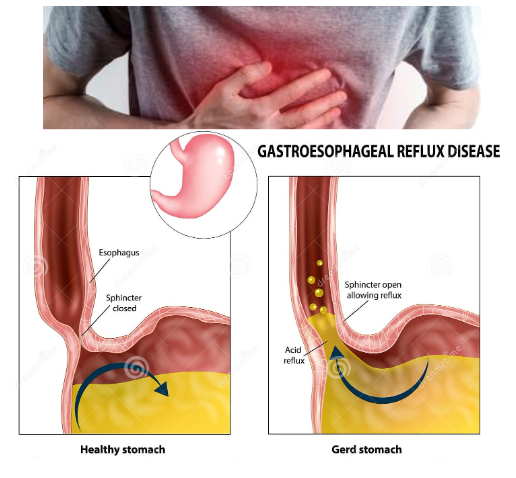
Gastroesophageal reflux disease (GERD) is a digestive disorder that occurs when stomach acid or, occasionally, stomach content, flows back into your esophagus — the tube that connects your throat to your stomach. This backwash (acid reflux) can irritate the lining of your esophagus, leading to symptoms and sometimes complications.
Causes
GERD is primarily caused by the dysfunction of the lower esophageal sphincter (LES), a muscle at the end of your esophagus that normally acts as a valve between the esophagus and stomach. When this valve fails to close properly or opens too often, stomach acid can flow back into the esophagus, causing GERD symptoms. Factors that can contribute to GERD include:- Obesity
- Hiatal hernia (when the stomach bulges up into the chest through an opening in the diaphragm)
- Pregnancy
- Smoking or exposure to secondhand smoke
- Certain medications (e.g., for asthma, calcium channel blockers for high blood pressure, antihistamines, painkillers, sedatives, and antidepressants)
Symptoms
The most common symptoms of GERD include:- Heartburn, a burning sensation in the chest that often occurs after eating and worsens when lying down
- Regurgitation of food or sour liquid (acid reflux)
- Difficulty swallowing
- A sensation of a lump in your throat
- Chronic cough
- Laryngitis
- New or worsening asthma
- Disrupted sleep
Diagnosis
GERD is often diagnosed based on the typical symptoms. Diagnostic tests can include:- Endoscopy: A doctor inserts a thin, flexible tube equipped with a light and camera (endoscope) down your throat to examine the inside of your esophagus and stomach.
- Esophageal pH monitoring: A monitor is inserted into your esophagus to measure when and how long stomach acid regurgitates there.
- Esophageal manometry: This test measures the rhythmic muscle contractions in your esophagus when you swallow.
- Barium swallow: After swallowing a barium solution, X-ray imaging is used to visualize your upper digestive tract.
Treatment
Treatment for GERD may involve lifestyle changes, medications, or occasionally surgery, depending on the severity of the condition:- Lifestyle changes: Avoiding foods that trigger reflux (like spicy or fatty foods), eating smaller meals, not lying down after a meal, losing weight, and stopping smoking.
- Medications: Over-the-counter antacids, H2 blockers, or proton pump inhibitors (PPIs) to reduce stomach acid.
- Surgical interventions: Procedures like Nissen fundoplication, where the top part of the stomach is wrapped around the lower esophagus to tighten the muscle and prevent reflux, or newer, less invasive treatments like LINX, a ring of tiny magnetic beads surgically placed around the esophagus to help keep it closed but still allow food to pass.
