Diabetes is a serious disease. It happens when the body does not make enough insulin or cannot use it well. This causes high levels of glucose (blood sugar) to build up in the blood. As a result, the body does not work like it should.
What Happens In Your Body?
- The food we eat is digested in our stomach. Here it is turned into glucose, or blood sugar.
- Blood takes glucose to our cells.
- Glucose must enter into our cells so that we can have energy. Glucose needs the help of insulin to do this.
- Glucose cannot enter into our cells if our body does not make enough insulin or if our cells cannot use the insulin well. This means the glucose will build up in the blood.
- People who have high levels of glucose in their blood have prediabetes or diabetes.
What Are The Symptoms?
The symptoms of type 2 diabetes develop over time. Some people have symptoms and others do not.
- Thirsty
- Frequent urination
- Feeling tired
- Hungry
- Unexplained weight loss
- Very dry skin
- Blurry vision
- “Pins and needles” feeling in feet
- Sores that do not heal
- Feeling irritable
Why Is Diabetes Dangerous?
Diabetes is a major risk factor for heart attack and stroke. Over time, high blood glucose damages the body. Diabetes can lead to blindness, amputation, kidney problems, and death.
Diabetes and heart disease are closely linked, and individuals with diabetes are at a higher risk of developing heart disease compared to those without diabetes. The relationship between the two conditions is complex, and several factors contribute to their association:
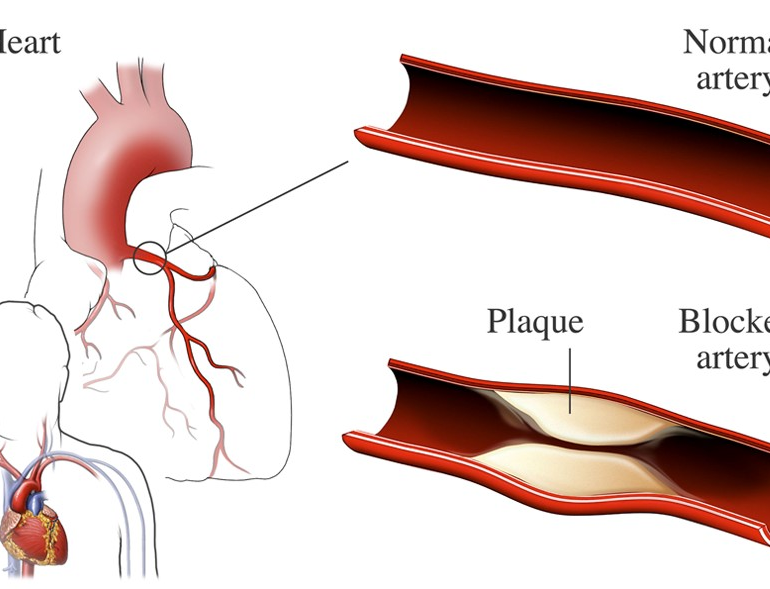
- Insulin Resistance: In type 2 diabetes, the body becomes resistant to the effects of insulin, leading to elevated blood sugar levels. Insulin resistance also affects lipid metabolism, leading to abnormal cholesterol levels and an increased risk of atherosclerosis, the buildup of plaque in the arteries.
- High Blood Sugar Levels: Elevated blood sugar levels can damage the blood vessels and nerves over time, increasing the risk of cardiovascular complications such as coronary artery disease, heart attack, and stroke.
- Hypertension: Diabetes is often associated with high blood pressure, which further strains the heart and increases the risk of heart disease.
- Dyslipidemia: Diabetes is commonly accompanied by abnormalities in lipid metabolism, including high levels of LDL (“bad”) cholesterol, low levels of HDL (“good”) cholesterol, and high levels of triglycerides, all of which contribute to the development of atherosclerosis and cardiovascular disease.
- Obesity and Metabolic Syndrome: Diabetes is often associated with obesity and metabolic syndrome, a cluster of conditions including high blood pressure, high blood sugar, abnormal cholesterol levels, and excess abdominal fat, all of which increase the risk of heart disease.
- Inflammation: Chronic inflammation, which is common in individuals with diabetes, plays a key role in the development and progression of atherosclerosis and cardiovascular disease.
- Diabetic Complications: Diabetes can lead to complications such as diabetic neuropathy (nerve damage), diabetic nephropathy (kidney damage), and diabetic retinopathy (eye damage), which can indirectly increase the risk of cardiovascular events.
- Lifestyle Factors: Unhealthy lifestyle habits such as poor diet, lack of physical activity, smoking, and excessive alcohol consumption are common risk factors for both diabetes and heart disease.
Managing diabetes effectively and controlling other risk factors for heart disease are essential for reducing the risk of cardiovascular complications. This may include lifestyle modifications (such as adopting a heart-healthy diet, regular exercise, smoking cessation, and stress management), medication management (such as glucose-lowering medications, blood pressure medications, and lipid-lowering medications), and regular medical check-ups to monitor and manage cardiovascular risk factors. Collaboration between healthcare providers, including primary care physicians, endocrinologists, cardiologists, and other specialists, is important for comprehensive care and prevention of cardiovascular complications in individuals with diabete
Benefits of Non-Starchy Vegetables for Blood Glucose Control
Eat more! You don’t often hear that when you have diabetes, but non-starchy vegetables are one food group where you can satisfy your appetite.
Vegetables are full of vitamins, minerals, fiber and phytochemicals—and with so few calories and carbohydrate, everyone can enjoy more!
There are two main types of vegetables—starchy and non-starchy. For this section, we are going to focus only on the non-starchy vegetables.
Choosing non-starchy vegetables
Choose fresh, frozen and canned vegetables and vegetable juices without added sodium, fat or sugar.
- If using canned or frozen vegetables, look for ones that say no salt added on the label.
- As a general rule, frozen or canned vegetables in sauces are higher in both fat and sodium.
- If using canned vegetables with sodium, drain the vegetables and rinse with water to decrease how much sodium is left on the vegetables.
For good health, try to eat at least three to five servings of vegetables a day. This is a minimum and more is better! A serving of vegetables is:
- ½ cup of cooked vegetables
- 1 cup of raw vegetables
Common non-starchy vegetables
The following is a list of common non-starchy vegetables:
- Amaranth or Chinese spinach
- Artichoke
- Artichoke hearts
- Asparagus
- Baby corn
- Bamboo shoots
- Beans (green, wax, Italian)
- Bean sprouts
- Beets
- Brussels sprouts
- Broccoli
- Cabbage (green, bok choy, Chinese)
- Cauliflower
- Celery
- Chayote
- Cucumber
- Daikon
- Eggplant
- Greens (collard, kale, mustard, turnip)
- Hearts of palm
- Jicama
- Kohlrabi
- Leeks
- Mushrooms
- Okra
- Onions
- Pea pods
- Peppers
- Radishes
- Rutabaga
- Salad greens (chicory, endive, escarole, lettuce, romaine, spinach, arugula, radicchio, watercress)
- Sprouts
- Squash (cushaw, summer, crookneck, spaghetti, zucchini)
- Sugar snap peas
- Swiss chard
- Tomato
- Turnips
- Water chestnuts
- Yard-long beans
1. Diabetes Fitness:
2. Diabetes Weight Management:
3. Diabetes and Your Health:
4. Diabetes Medication:
5. Diabetes Better Choices for Life Program:
6. Healthy Eating Tips:
7. Diabetes & Food:
8. Recipes from Diabetes Food Hub:
Link: