Cardiomyopathy refers to a group of diseases that affect your heart muscle, making it harder for your heart to pump blood efficiently throughout your body. There are different types of cardiomyopathy, each with its own cause and characteristics.
Here’s a breakdown of cardiomyopathy:Types of Cardiomyopathy:
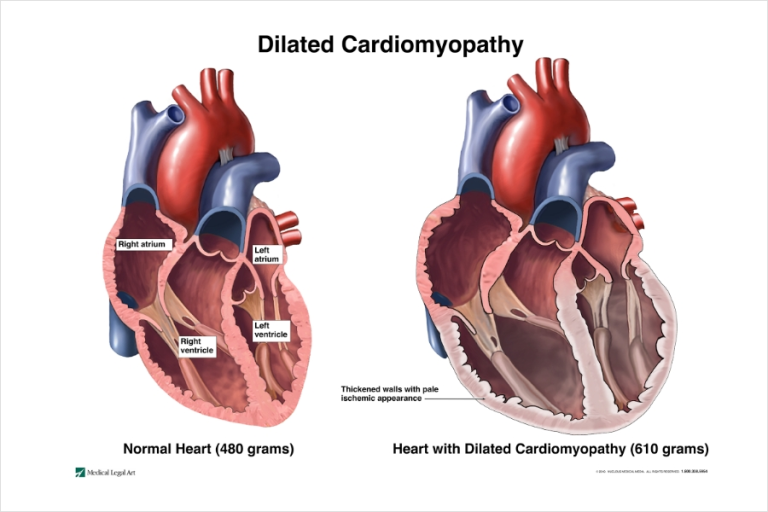
- Dilated cardiomyopathy: The most common type, where the heart’s ventricles (lower chambers) become enlarged and weakened, compromising their pumping function.
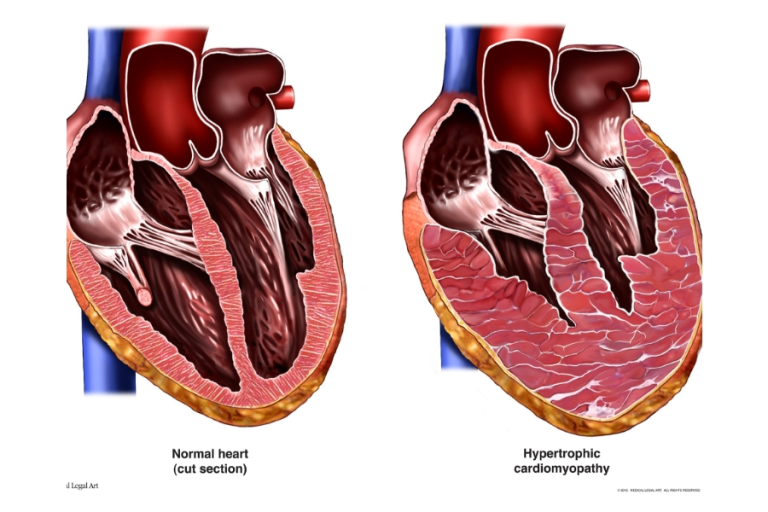
- Hypertrophic cardiomyopathy: In this type, the heart muscle thickens abnormally, which can obstruct blood flow or cause abnormal heart rhythms.
- Restrictive cardiomyopathy: The heart muscle becomes stiff and inflexible, hindering its ability to fill with blood between beats.
- Arrhythmogenic right ventricular cardiomyopathy (ARVC): This rare condition affects the heart’s right ventricle, increasing the risk of irregular heartbeats.
- Peripartum cardiomyopathy: A rare but serious condition that develops in some women in the later stages of pregnancy or shortly after delivery.
Causes:
The causes of cardiomyopathy can vary depending on the type:- Dilated cardiomyopathy: Often idiopathic (unknown cause), but viral infections, genetic factors, certain medications, and pregnancy complications can contribute.
- Hypertrophic cardiomyopathy: Usually caused by genetic mutations passed down through families.
- Restrictive cardiomyopathy: Can be caused by amyloidosis (abnormal protein deposits in the heart), hemochromatosis (iron overload), or exposure to certain toxins.
- ARVC: Primarily caused by genetic mutations.
- Peripartum cardiomyopathy: The exact cause is unknown, but hormonal changes and pregnancy complications might be involved.
Symptoms:
Early stages of cardiomyopathy may not cause any noticeable symptoms. As the condition worsens, common symptoms include:- Fatigue and shortness of breath, especially during exertion
- Swelling in the ankles and legs (edema)
- Rapid or irregular heartbeats (palpitations)
- Chest pain or tightness
- Lightheadedness or dizziness
Diagnosis:
Diagnosis of cardiomyopathy often involves a combination of tests such as:- Medical history and physical exam
- Electrocardiogram (ECG) to assess heart rhythm and electrical activity
- Echocardiogram to evaluate the heart’s structure and pumping function
- Chest X-ray to check for lung congestion
- Blood tests to rule out other conditions
Treatment:
There’s no cure for cardiomyopathy, but treatment can help manage symptoms, slow disease progression, and improve your quality of life. Treatment options may include:- Medications like diuretics to reduce fluid buildup, ACE inhibitors or ARBs to lower blood pressure, and beta-blockers to control heart rate.
- Lifestyle modifications like a healthy diet, regular exercise, weight management, and stress reduction.
- In some cases, medical devices like pacemakers or implantable cardioverter-defibrillators (ICDs) might be needed to regulate heart rhythm.
- Advanced procedures like surgical procedures or heart transplant might be considered in severe cases.
Living With Cardiomyopathy:
While cardiomyopathy is a serious condition, early diagnosis and proper management can significantly improve your outlook. Regular doctor visits, adherence to treatment, and a healthy lifestyle are crucial for managing cardiomyopathy and living a fulfilling life.Here are some additional points to remember:
- Cardiomyopathy can affect people of all ages, although some types are more common in certain age groups.
- The specific cause and severity of cardiomyopathy can vary depending on the type.
- Early detection and treatment are essential for managing cardiomyopathy and preventing complications like heart failure.
